|
Further, etiology of the liver disease as a factor was removed from the model, as this did not impact mortality amongst patients with end-stage liver disease awaiting LT. 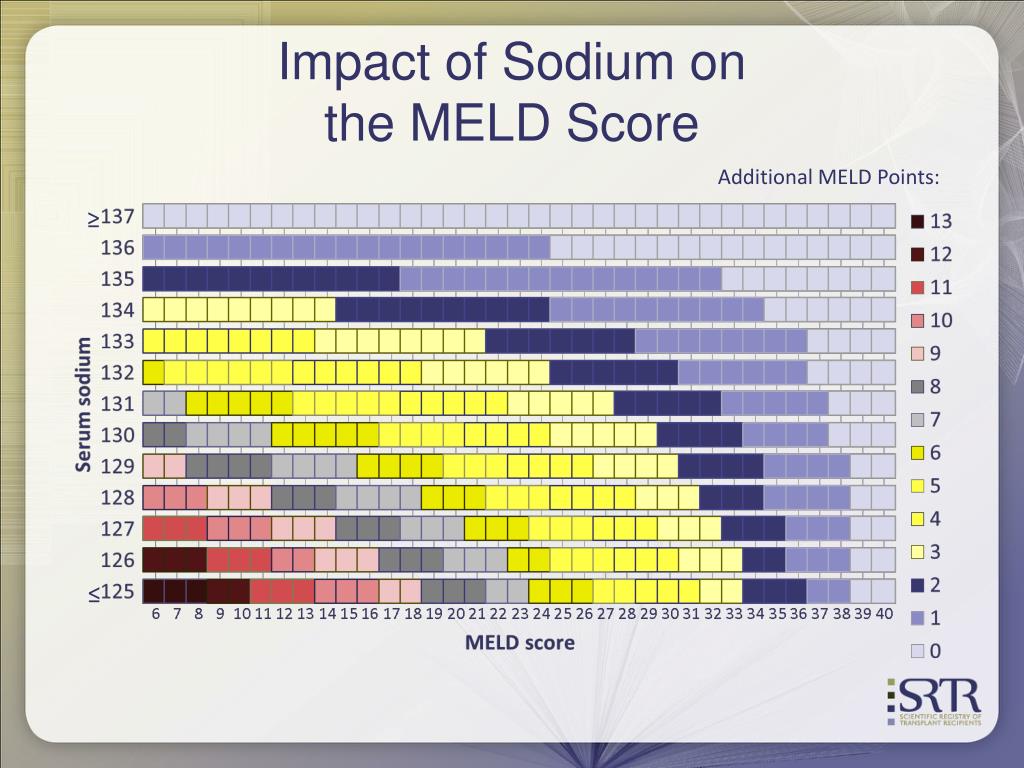
7, 8 Other changes made to the score by the UNOS were: capping serum creatinine at 4 mg/dl, capping the score at 40, and setting the lower limit for each component of the score to 1 in order to avoid negative scores. This allowed wider acceptability of the score keeping the same abbreviation of MELD. With the acceptance of this score by the UNOS for organ allocation, the model was renamed as model for end-stage liver disease. The score was initially named as Mayo model for end-stage liver disease (MELD) score reflecting the institution where the score was developed. 5, 6 As the score was objective and could predict mortality at 3 months with higher accuracy than the CTP score, allocation of livers for transplantation became MELD based, de-emphasizing the concept of waiting time. 4 The model was later shown to quite accurately predict 3 months mortality amongst patients with chronic end-stage liver disease awaiting LT. MELD score was developed by a group of researchers at the Mayo Clinic initially as a model to predict survival following transjugular intrahepatic portosystemic (TIPS) for refractory variceal bleeding or refractory ascites. That is, the patient most at risk for mortality would be at the highest priority for organ allocation. 3 This score changed the policy of organ allocation not only upholding the concept of “patient comes first” but also “sickest patient comes first”. 2ĭevelopment of the Model for End-stage Liver Disease Score and Adoption by the United Network for Organ Sharing for Liver Allocationįebruwas a historical day when the MELD score was adopted and approved by the United Network for Organ Sharing (UNOS) as a score to allocate organs for patients awaiting liver transplantation (LT) in the United States. In 1998, the Institute of Medicine mandated that patients be allocated organs based on their disease severity and risk of death rather than on waiting time. Organ allocation for patients with end-stage liver disease (ESLD), however, largely depended on waiting time on the list. CTP score introduced to some extent the concept of ‘sicker patient first’ with the introduction of status 1A for patients with fulminant hepatic failure, primary non-function or hepatic artery thrombosis within 7 days of transplantation, and decompensated Wilson's disease. Subjective parameters vary with use of diuretics or paracenteses for ascites and use of lactulose for encephalopathy. 1 CTP score is based on severity of 3 objective (serum albumin, serum bilirubin, and prothrombin time) and 2 subjective (ascites and encephalopathy) parameters. In 1996, a consensus conference mandating need for minimal criteria for listing the patients for liver transplantation (LT) introduced the Child–Pugh–Turcotte (CTP) score for liver allocation. This approach had the potential of ‘gaming’ the system by keeping the patients in ICU in order to be transplanted. Until, a better score is developed, liver allocation would continue based on the currently used MELD score.Īllocation of organs for liver transplantation in the United States in the 1980s and early 1990s was prioritized based on the level of care required by the patient: hospitalized patients in the intensive care unit, hospitalized patients on the regular floor, and outpatient care. Over the last decade, many efforts have been made to further improve and refine MELD score. Although, MELD score is closest to the ideal score, there are some limitations including its inaccuracy in predicting survival in 15–20% cases. MELD score has also been shown to be accurate predictor of survival amongst patients with alcoholic hepatitis, following variceal hemorrhage, infections in cirrhosis, after surgery in patients with cirrhosis including liver resection, trauma, and hepatorenal syndrome (HRS). 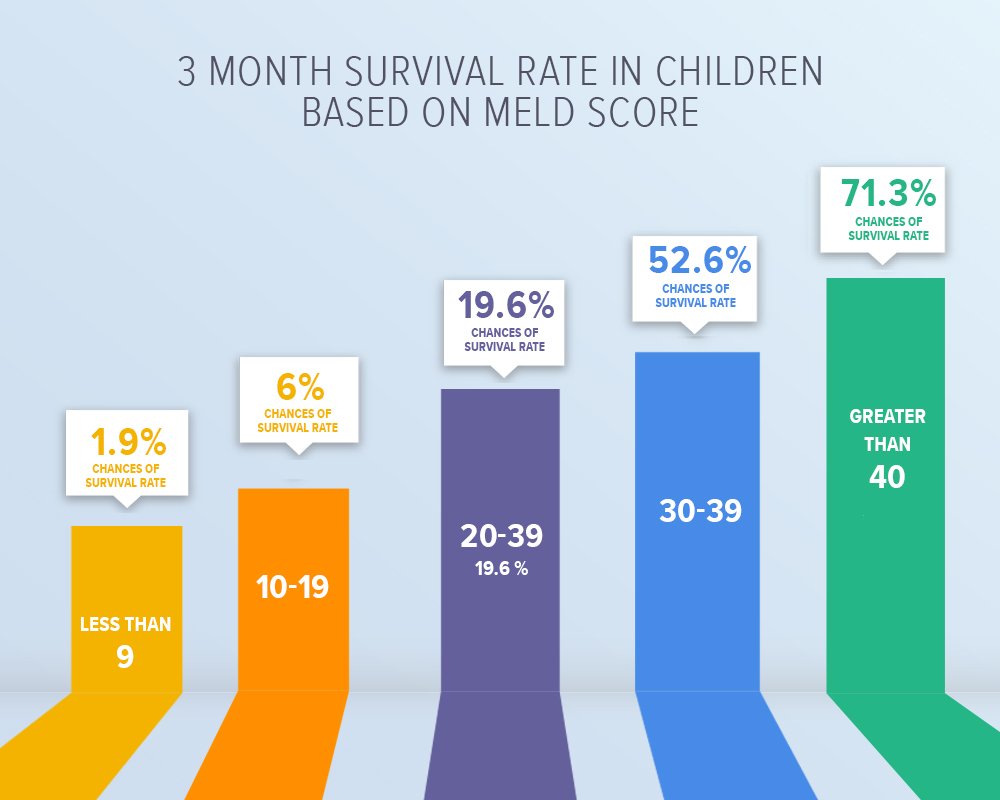
Since 2002, MELD score using 3 objective variables (serum bilirubin, serum creatinine, and institutional normalized ratio) has been used worldwide for listing and transplanting patients with end-stage liver disease allowing transplanting sicker patients first irrespective of the wait time on the list. Model for end-stage liver disease (MELD) score, initially developed to predict survival following transjugular intrahepatic portosystemic shunt was subsequently found to be accurate predictor of mortality amongst patents with end-stage liver disease.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
